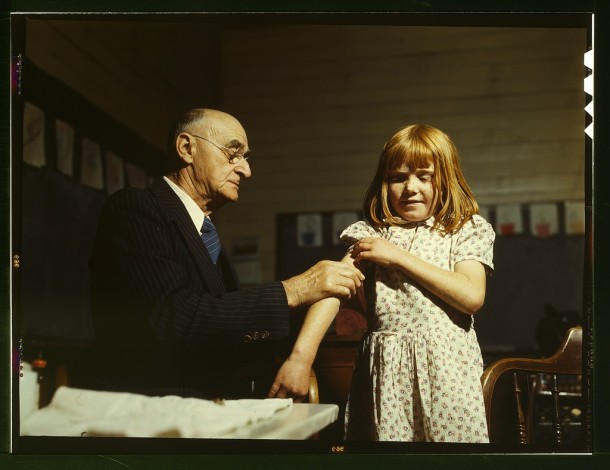
Vaccines are “about the closest thing we have to a miracle in modern medicine.” These are the words of Sue Desmond-Hellman, CEO of the Bill and Melinda Gates Foundation. The scientific community concurs. Experts recently ranked vaccines number eight among The 50 Greatest Breakthroughs Since the Wheel—ahead of inventions like the Internet, sanitation, and the automobile.
Vaccines are a major step in human progress: they prevent the deaths of 2-3 million children every year, and since the 1950s have helped increase global life expectancy by more than twenty years. These remarkable achievements are made possible by harnessing the internal powers of the human body. Vaccines enable the immune system to fight against disease causing bacteria or viruses called pathogens. The material in a vaccine that kick starts the immune response is a weakened or dead part of a specific pathogen that makes us sick. Exposure to pathogens through vaccination primes the immune system to recognize, remember, and attack the bacteria and viruses that cause a wide range of life-threatening diseases. Once the body has a memory of a pathogen, either from receiving a vaccine or recovering from a previous infection, a person has a high degree of protection from getting sick with that specific pathogen. This process of creating immunity and immune memory is called immunization.
Vaccinations today protect against many diseases, but this was not always the case. For many years smallpox was the only disease that could be prevented by inoculation, the term for intentionally exposing the body to a pathogen to achieve immunization. An early form of inoculation against smallpox, called variolation, was practiced for centuries in China, India, Turkey, and Africa and became popular in the United States and Europe in the 1700s. People would inhale or insert under the skin the powdered scabs and fluid from the smallpox sores of people who survived milder forms of the disease. Though variolation offered a degree of personal protection, most people were mildly ill for a few days then recovered, it was not without risk. Variolated individuals could still transmit smallpox to their families and communities and about 1-2% of those who were variolated contracted severe smallpox and died.
It wasn’t until the late 1700s that the modern vaccine was born when British physician Edward Jenner found an effective method to protect against smallpox. The procedure was similar to variolation, but Jenner, with the help of his cow (fondly named Blossom), discovered that humans could more safely achieve immunity to smallpox by being exposed to fluid from cowpox sores. Both smallpox and cowpox are caused by viruses that are very closely related, and the viruses are similar enough that the body can achieve immunity to smallpox by learning to attack the cowpox virus. Jenner called his procedure “vaccination”, from vaca – the Latin word for cow.
The practice of smallpox vaccination expanded during the 1800s, and vaccine development progressed as the early vaccines for rabies, typhoid, diphtheria, and tuberculosis were developed in the early 1900s. The emergence of vaccination programs as we would recognize them today began in the 1950s and 1960s when mass vaccination began to prevent polio and measles in the U.S. Another milestone in vaccine history was in 1974 when the World Health Organization (WHO) began the Expanded Program on Immunization (EPI) to vaccinate children all over the world against such ubiquitous diseases as diphtheria, polio, tuberculosis, pertussis, measles, and tetanus. Vaccine development proceeded slowly thereafter, but has recently begun to accelerate, and today we have vaccines that protect against a multiplicity of infectious diseases, including chickenpox, meningitis, pneumonia, human papilloma virus, and rotavirus. There are several promising vaccine candidates in development and the world may very soon have vaccines to prevent malaria and dengue fever as well as HIV and Ebola. The WHO currently recommends that children under one year of age receive nine different vaccines, with the inclusion of a number of other vaccines under active consideration. Additionally, the WHO’s Global Vaccine Action Plan 2011-2020 promotes vaccines beyond infancy, underscoring the importance of adolescent vaccination against the human papilloma virus, which causes several cancers, and of maternal vaccination against tetanus and diphtheria.
This expansion of vaccines is a giant leap forward for public health, but many children still cannot and do not receive the recommended vaccines for various reasons that will be covered in subsequent entries in this series. According to the WHO, 1.5 million children still die each year from vaccine preventable diseases and in 2013 there were over 20 million children who did not receive the recommended doses of a combination vaccine to prevent diphtheria, tetanus, and pertussis. Well over two thirds of these children live in ten countries, most notably in Africa and Asia, which highlights the inequities in access to vaccines due to poor infrastructure and communications as well as challenges with health system capacities, logistics, and service quality.
In more developed countries, a contrasting scenario exists with some parents choosing not to vaccinate their children over concerns, often due to misinformation, about vaccine related health complications and suspicion toward the vaccine industry.
The scientific and public health communities have accomplished much with respect to the development and delivery of vaccines. However, a lack of resources, weak political commitment and instability, and vaccine abstention threaten our ability to achieve global goals for vaccination coverage and disease control. On the bright side, the global health community is taking positive steps to allocate more resources to vaccine delivery, and is developing a potent new battery of vaccines. In this way, it is positioning itself to avert a great deal of avoidable suffering and premature death and to drive further gains in human health and well-being.